Blood Lead Levels in Children
What Do Parents Need to Know to Protect Their Children?
Protecting children from exposure to lead is important to lifelong good health. Even low l evels of lead in blood have been shown to affect IQ, ability to pay attention, and academic achievement. And effects of lead exposure cannot be corrected. The most important step parents, doctors, and others can take is to prevent lead exposure before it occurs
Update on Blood Lead Levels in Children:
Children can b e given a blood test to measure the level of lead in their blood. Until recently, children were identified as having a blood lead level of concern if the test result is 10 or more micrograms per deciliter of lead in blood. Experts now u se a new level based on the U.S. population of children ages 1-5 years who are in the top 2.5% of children when tested for lead in their blood (when compared to children who are exposed to more lead than most children). In the past, blood lead level tests below 10 micrograms per deciliter of lead in blood may, or may not, have been reported to parents. The new, lower value means that more children likely will be identified as having lead exposure allowing parents, doctors, public health officials, and communities to take action earlier to reduce the child’s future exposure to lead. What has not changed is the recommendation fo r when to use medical treatment for children. These new recommendations do not change the recommendation that chelation therapy be considered when a child is found with a test result of greater than or equal to 45 micrograms per deciliter of lead in blood.
Actions for Parents :
Parents can ta ke simple steps to make their homes more lead-safe.
Talk to your local health department about testing paint and dust in your home for lead if you live in a home built before 1978. Common home renovation activities like sanding, cutting,
and demolition can c reate hazardous lead dust and chips by disturbing lead-based paint. These can b e harmful to adults and children. Renovation ac tivities should be performed by certified renovators who are trained by EPA-approved training providers to follow l ead-safe work practices. Learn more at EPA’s Renovation, Repair, and Painting rule. If you see paint chips or dust in windowsills or on floors because of peeling paint, clean these areas regularly with a wet mop. Wipe your feet on mats before entering the home, especially if you work in occupations where lead is used. Removing your shoes when you are entering the home is a good practice to control lead. Remove recalled toys and toy jewelry from children.
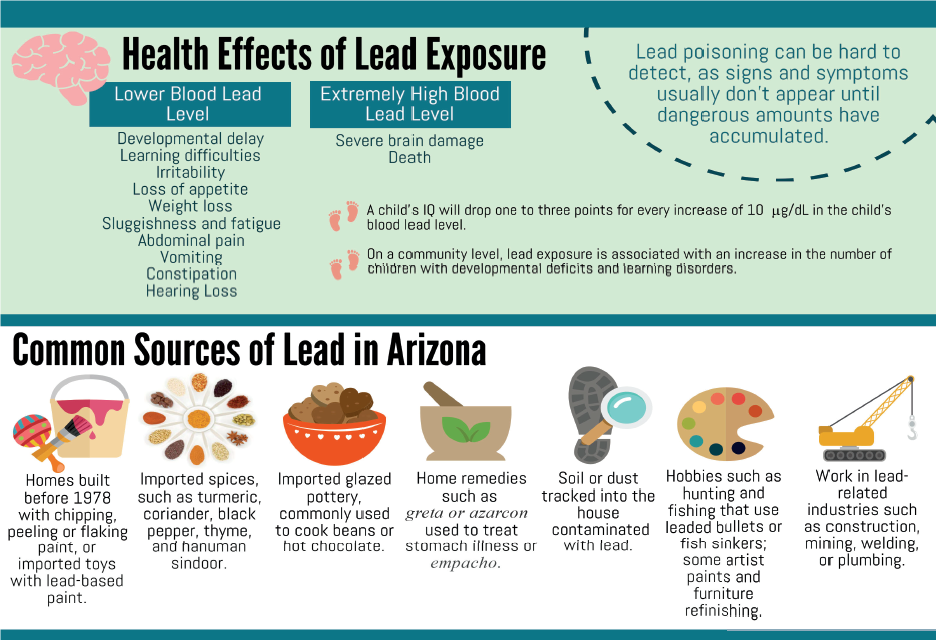
Lead can be found in a variety of sources. These include: paint in homes built before 1978. water pumped through leaded pipes. imported items including clay pots. certain consumer products such as candies, make -up and jewelry. certain imported home remedies.
Effect of a Different Blood Lead Level
In the past, blood lead level tests below10 micrograms per deciliter may, or may not, have been reported to parents. Identifying a child’s blood lead equal to or above 5 micrograms per deciliter means more parents should learn that their child has an elevated blood lead level. Even though no medical treatment is recommended for children with blood lead levels lower than 45 micrograms per deciliter, parents will know they need to learn about sources of lead exposure and find out if one or more unrecognized sources of lead are present in their home. Parents then can follow the Centers for
Disease Control and Prevention (CDC)’s recommendations to control exposure to lead.
No changes are recommended to the existing CDC guidelines for the evaluation and treatment of children requiring chelation (those with BLLs ≥ 45 micrograms per deciliter).
New Recommendations to Define Elevated Blood Lead Levels
In January 2012, a committee of experts recommended that the CDC change its “blood lead level of concern.” The recommendation was based on a growing number of scientific studies that show that even low b lood lead levels can c ause lifelong health effects. The committee recommended that CDC link lead levels to data from the National Health and Nutritional Examination Survey (NHANES) to identify children living or staying for long periods in environments that expose them to lead hazards. This new level is based on the population of children aged 1-5 years in the U.S. who are in the top 2.5% of children when tested for lead in their blood. Currently, that is 5 micrograms per deciliter of lead in blood. CDC’s “blood lead level of concern” has been 10 micrograms per deciliter. The n ew v alue means that more children will be identified as having lead exposure earlier and parents, doctors, public health officials, and communities can ta ke action ear lier. The committee also said, as CDC has long said, that the best way to protect children is to prevent lead exposure in the first place.